

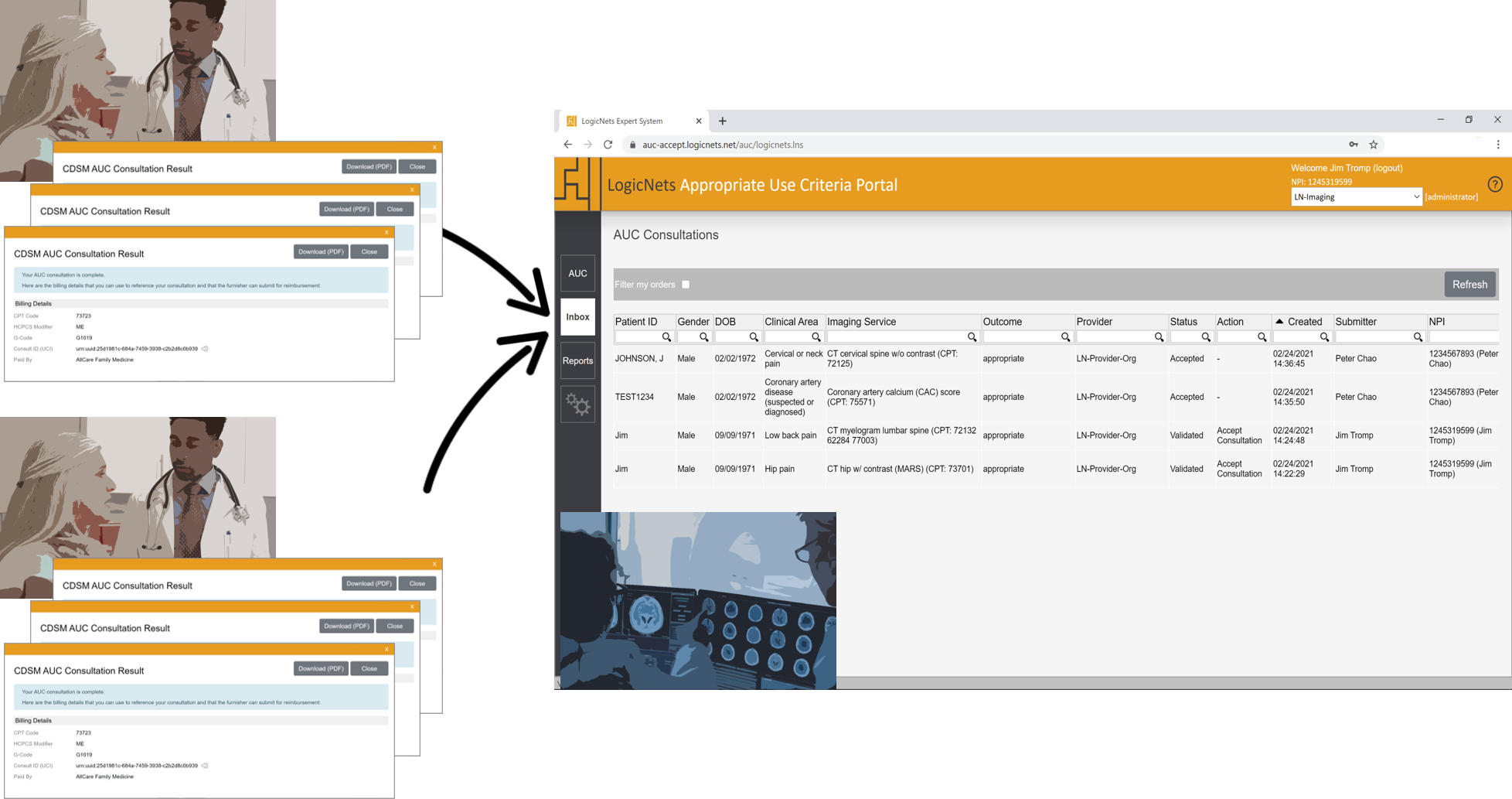
The AUC Solution is not simply a CDS mechanism – its browser-based portal can help furnishing providers securely aggregate and organize AUC consultation results from your referring physicians as well as your internally ordered procedures. Your external partners generate AUC consultations with their own AUC Solution instances and then direct the results to you electronically for processing. Your AUC Portal inbox will show these consultations and allow you to quickly review and advise the partner whether the validation was accepted or not. The inbox can aggregate activity from any number of partner organizations, but it allows you to easily filter, list, review, and process any subset of AUC consultation results.
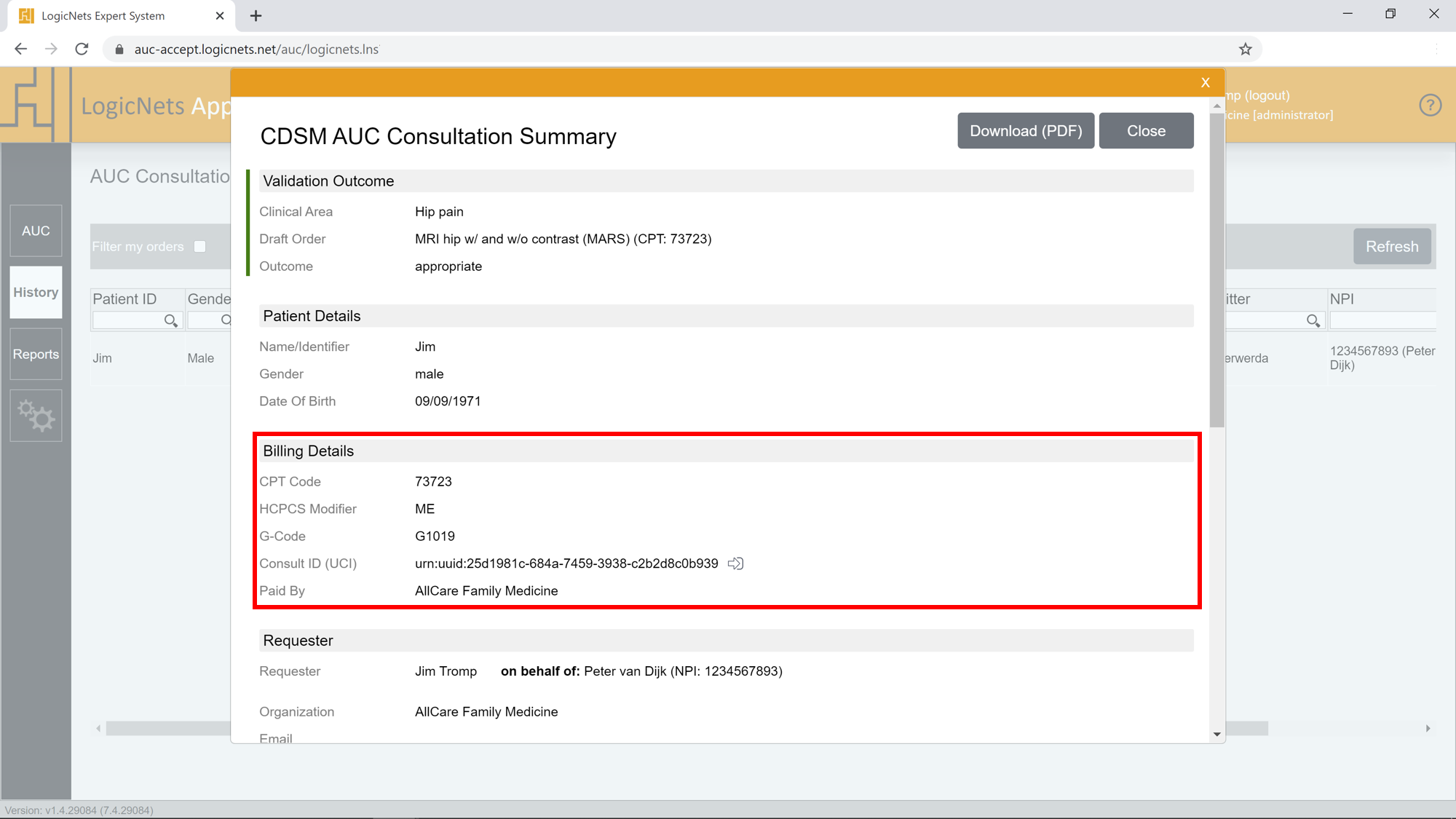
Collaborating on AUC validation through the AUC Portal ensures that you will always receive accurate billing and reimbursement information. Your referrers always submit complete results as they finalize and make their AUC consultations available to you from the Portal. And all the information required by CMS is presented for your review in a clear and complete form so that you can transfer it to your billing system in a few clicks. Once you have ensured that your reimbursement process is complete, you can accept the referrer’s submission to inform them through their AUC Portal instance that the order will be processed.
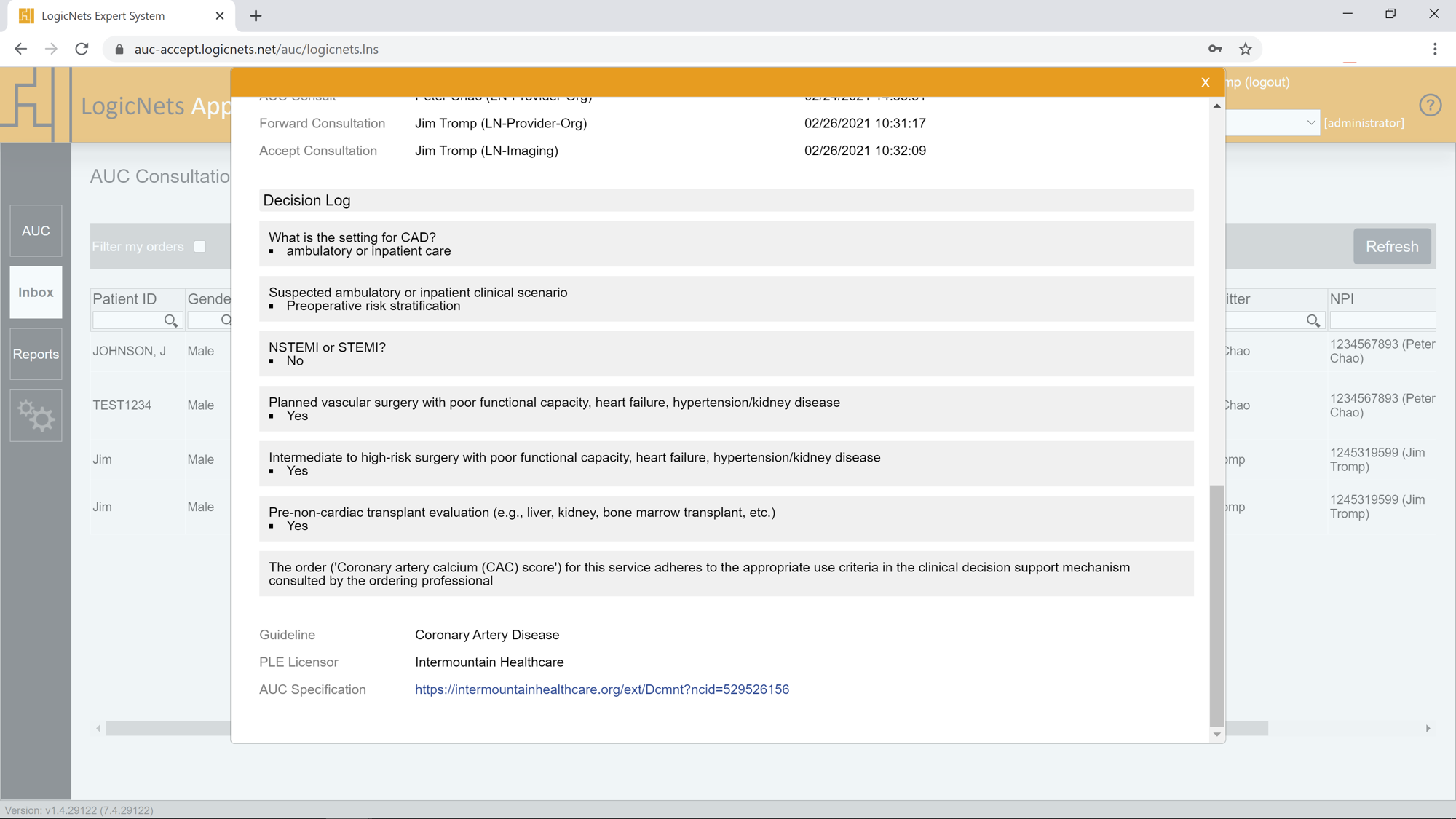
The consultation results always include a complete copy of the AUC consultation decision log – the audit trail of patient scenario information provided by the referring physician that led to the AUC results that you have received. Gone are the days when you had to call the referring provider’s office to understand why a particular order was requested. You can recognize edge cases or determine if special advise is needed. You can also see if the referrer has elected not to follow the AUC guidance and you can then determine if the order should be processed prior to potentially bearing the cost of non-reimbursement.
The LogicNets AUC Portal enables a powerful level of secure cloud-based collaboration between imaging centers and their referring provider partners. The AUC Portal itself is free and your staff and referring partners can easily signup for their own accounts and either set up or request access under their respective organizations.
You can then allow users from your connected referring providers to see and select your organization from their list of available imaging center partners to indicate that you will be processing their order. When the ordering professional selects your imaging center, the AUC consultation results are “forwarded” to the inbox of your authorized staff so that they can open the new request up, review the AUC validation, and indicate that is acceptable.
As part of this process, you can even sponsor the AUC validation for selected partners.
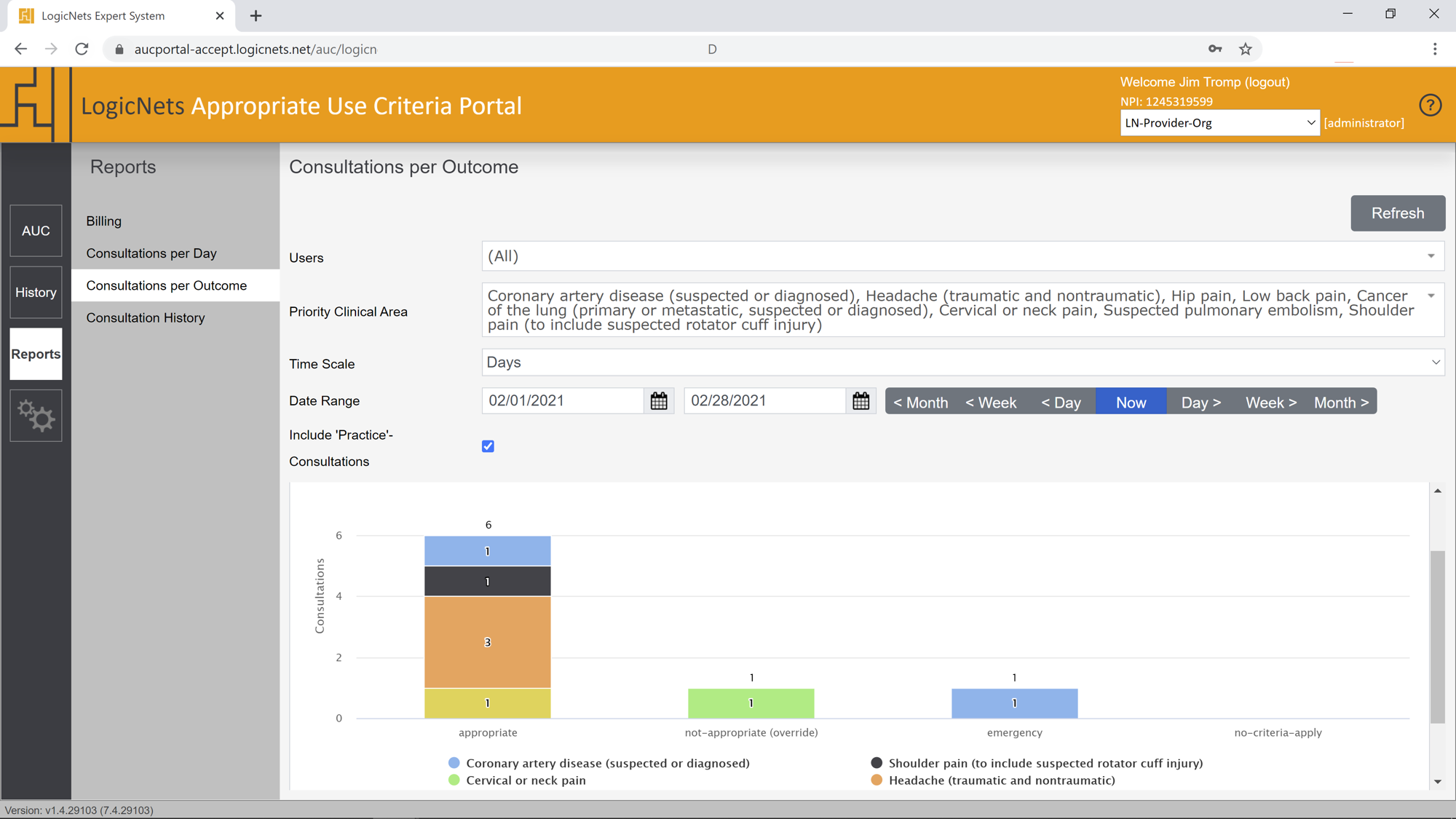
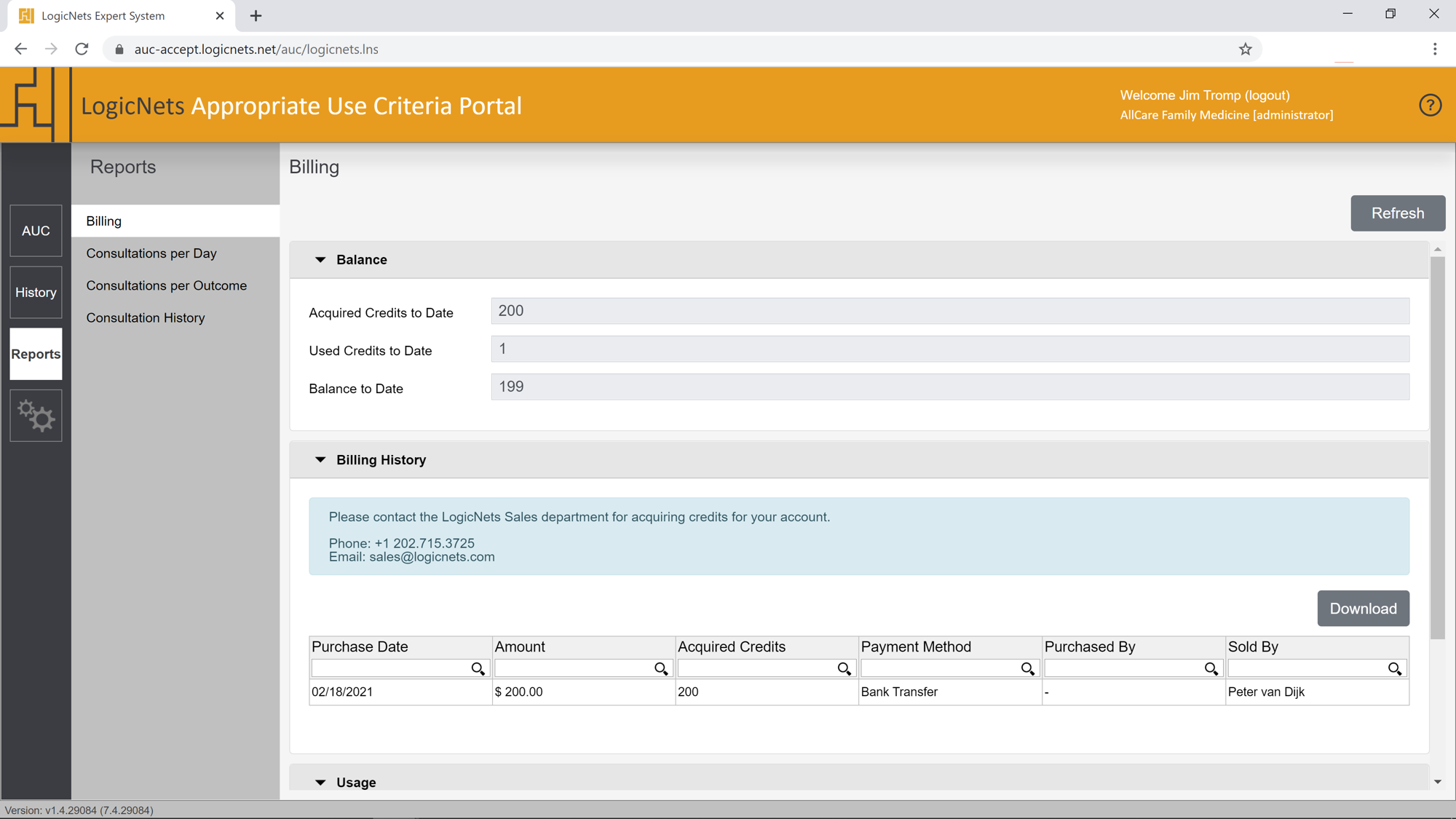
The AUC Portal’s graphic and tabular reporting module ensures that both you and your organization have a clear view of the AUC consultations that support reimbursement for Medicare and Medicaid patients. The reports show the distribution of both outcomes and clinical priority areas for the orders you received from your referrers connected via the AUC Portal. They allow you to quantify and gain insight into your PAMA compliance and approval and reimbursement processes. The Reporting application can also be used for auditing specific consultations. The user can specify the UCI of any consultation and the system will display a complete summary of the consultation.